Obesity, which is a worldwide epidemic, has vast metabolic effects on individuals suffering from the disorder which may shorten your life span and cause an increase in severe complications, some including type 2 diabetes, hypertension, and cardiovascular disorders/disease.
In a recent paper by Schmidt, et al., researchers have investigated the immunoregulatory effects of type 2 T helper (Th2) cells in an environment characterised by significantly high fat stores and malnutrition (Figure 1). T-cell responses can be dysregulated in individuals suffering with obesity. This dysregulation favours the inflammatory Th1 response over the Th2. A higher case of severe clinical illness has been reported in patients with SARS-CoV-2 infection who are obese (READ MORE).
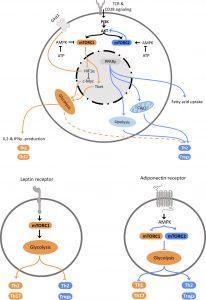
Figure 1 Regulation of Th2 metabolism. Top: Schematic representation of intracellular mechanisms affecting T helper cell polarization. Central elements influencing cellular polarization include mTORC1 and mTORC2, which are regulated by PI3K/Akt and AMPK, PPARγ and HIF-1α. These pathways regulate utilization of glycolysis, which promotes pro-inflammatory subset differentiation, or fatty acid oxidation and lipolysis that promote anti-inflammatory Th2 and Treg differentiation. Bottom: Schematic representation how the adipokines leptin (left) and adiponectin (right) promote T helper cell subset polarization via regulation of metabolic pathways (Schmidt, et al., 2022).
Regulation of metabolism both locally and in the periphery is essential for the maintenance of an effective CD4 T-cell population. Shifts in our metabolism are induced by intrinsic and extrinsic factors. In the case of Th2 cells, they are susceptible to the availability of and type of nutrients. Th2 cells are also inhibited by the activation of mTORC1 and leptin secretion, whilst being activated or improved by adiponectin and APMK.
In the case of oese individuals, the environment inside the body is nutrient rich and thus provides sufficient energy for T-cells, especially in the form of fatty acids, in adipose tissue. Proliferation of Th1 cells in adipose tissues inhibits Th2 cell function and proliferation, leading to an imbalance in the Th1-Th2 cell ratio. This could result in a loss of cells that are protective against insulin resistance and systemic inflammation.
In short, “obesity disrupts the homeostatic environment in favour of a pro-inflammatory Th1 bias, the step forwards, while Th2 cells cause a step back from obesity.”
Journal article: Schmidt, V., et al., 2022. Obesity-Mediated Immune Modulation: One Step Forward, (Th)2 Steps Back. Frontiers in Immunology.
Summary by Stefan Botha










