Introduction
Mycobacterium tuberculosis infection is currently treated using either first-line therapeutic drugs or second-line therapeutic drugs. The first-line therapeutic drugs are the most effective and least toxic for use in the treatment of TB, while the second-line therapeutic drugs are less effective, more expensive and have higher toxicities. They are however, essential for the treatment of drug resistant forms of the bacteria (MDR-TB).
In this section we detail the various drugs used in first-line treatment as well as the second-line therapeutic drugs that are currently available.
First-Line Therapeutic Drugs
There are 5 essential drugs in use in the treatment of Mycobacterial infections and they are referred to as first-line therapeutic drugs. The mechanism of action of each of the first-line drugs is shown in greater detail for: streptomycin, rifampicin, isoniazid, pyrazinamide and ethambutol.
Download First-line TB Drug Action Guide
 These drugs act on two key properties of mycobacterial cell growth:
These drugs act on two key properties of mycobacterial cell growth:
- The first is the synthesis of the cell wall of the bacterium
- The second is the synthesis of bacterial proteins.
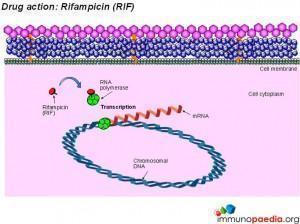
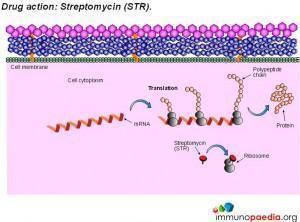
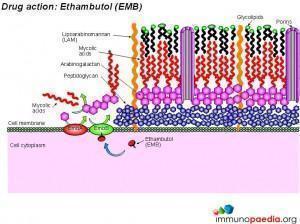
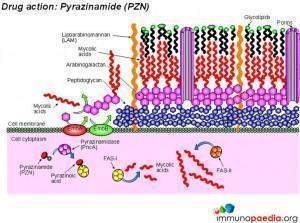
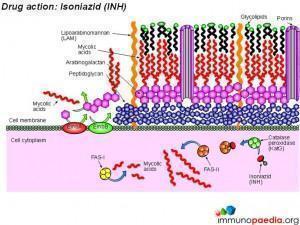 Three drugs (isoniazid, pyrazinamide and ethambutol) all interfere with the synthesis of key components of the bacterial cell wall , namely arabinogalactan and mycolic acids. Streptomycin and rifampicin interfere with protein synthesis by inhibiting the transcription of messenger RNA and the translation of messenger RNA to produce bacterial proteins. These drugs are the most effective and least toxic for use in treatment of TB.
Three drugs (isoniazid, pyrazinamide and ethambutol) all interfere with the synthesis of key components of the bacterial cell wall , namely arabinogalactan and mycolic acids. Streptomycin and rifampicin interfere with protein synthesis by inhibiting the transcription of messenger RNA and the translation of messenger RNA to produce bacterial proteins. These drugs are the most effective and least toxic for use in treatment of TB.
 There are second-line therapeutic drugs which are less effective, more expensive and with higher toxicity, but are essential for the treatment of drug resistant forms of mycobacteria.
There are second-line therapeutic drugs which are less effective, more expensive and with higher toxicity, but are essential for the treatment of drug resistant forms of mycobacteria.
Second-Line Therapeutic Drugs
Compared to the first-line drugs, the second-line therapeutic drugs used for the treatment of Mycobacterium tuberculosis infection are less effective, more expensive and have higher toxicities. They are however, essential for the treatment of drug resistant forms of the bacteria (MDR-TB).
Download Second-line TB Drug Action Guide
 The mechanism of action of each of the second-line drugs is shown in greater detail for: Ethionamide, D-cycloserine, Ciproflaxin, Ofloxacin, Kanamycin, Amikacin, Viomycin and Capreomycin. The action of these drugs is against cell wall biosynthesis, DNA supercoiling and protein synthesis in Mycobacterium tuberculosis.
The mechanism of action of each of the second-line drugs is shown in greater detail for: Ethionamide, D-cycloserine, Ciproflaxin, Ofloxacin, Kanamycin, Amikacin, Viomycin and Capreomycin. The action of these drugs is against cell wall biosynthesis, DNA supercoiling and protein synthesis in Mycobacterium tuberculosis.
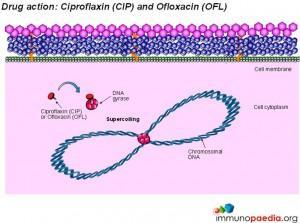
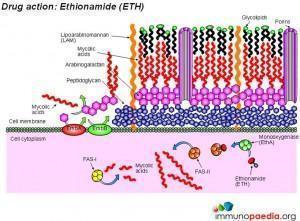
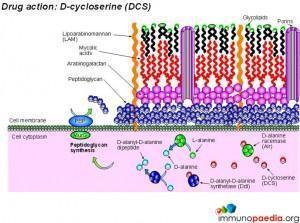
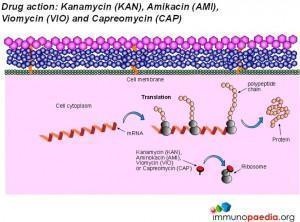 Ethionamide and D-cycloserine interfere with cell wall biosynthesis by inhibiting mycolic acid synthesis and peptidoglycan synthesis, respectively. Ciproflaxin and Ofloxacin are fluoroquinolone drugs that inhibit DNA supercoiling by inhibiting the DNA gyrase enzyme. Kanamycin and Aminokacin are aminoglycoside drugs that interfere with protein synthesis by inhibiting the action of ribosomes. Similarly, Viomycin and Capreomycin are peptide drugs that also inhibit the action of ribosomes.
Ethionamide and D-cycloserine interfere with cell wall biosynthesis by inhibiting mycolic acid synthesis and peptidoglycan synthesis, respectively. Ciproflaxin and Ofloxacin are fluoroquinolone drugs that inhibit DNA supercoiling by inhibiting the DNA gyrase enzyme. Kanamycin and Aminokacin are aminoglycoside drugs that interfere with protein synthesis by inhibiting the action of ribosomes. Similarly, Viomycin and Capreomycin are peptide drugs that also inhibit the action of ribosomes.