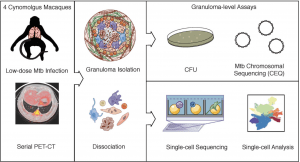
Study design: Cynomolgus macaques (n=4) were infected with a low-dose inoculum of Mtb (Erdman strain) and serial PET-CT scans were performed at 4, 8, and 10 weeks post-infection with the final scan used as a map for lesion identification at necropsy. Individual granulomas were excised and homogenized. CFU and CEQ assays were performed on all granulomas (top right) and 26 individual granulomas across 4 animals were randomly selected at necropsy for Seq-Well assays (bottom right). Source: Gideon et al., Pre-print
Tuberculosis (TB), second only to COVID-19, is one of the leading causes of death due to a single infectious agent. Approximately a quarter of the global population is estimated to have Mycobacterium tuberculosis infection (TB etiological agent). However, only 5-10% of infected individuals progress to disease. This suggests that there are mechanisms of protective immunity that we do not fully understand yet. On the 8th of March, the IUIS-Immunopaedia-Frontiers webinar series hosted tuberculosis immunologist Dr JoAnne Flynn. In honour of World TB Day on the 24th of March, we shall provide three summaries highlighting findings shared during Dr Flynn’s talk.
Dr Flynn began her talk with a brief overview of how M.tb infection can lead to the development of granulomas (structured organisation of cells that aim to contain M.tb replication). The majority of Dr Flynn research utilises non-human primate (NHPs) models, specifically cynomolgus (latent to active TB) and rhesus (almost always active TB) macaques, that represent the full spectrum of human TB infection and disease. In this summary, we shall focus on findings presented that relate to natural infection.
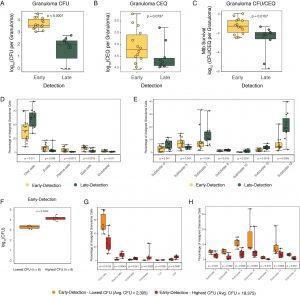
Association of cell type proportions with timing of granuloma formation A-C. CFU log10 values(A), CEQ log10 values (B) and relative bacterial survival (CFU/CEQ)(C) for granulomas grouped by time of initial observation by PET-CT imaging. Early detection (yellow): those identified at 4 weeks p.i.; Late detection (green): those identified at 10 week p.i.. D,E. Canonical cell type clusters (D) and T/NK subclusters (E) that are significantly different between early and late detection granulomas. See Table S10 for full data. F. Early (4 week) detection granulomas comparing lowest CFU (n=6) and highest CFU (n=6) granulomas. G, H. Relationship between the abundance of canonical cell types (G) and T/NK subclusters (H) with bacterial burdens among low CFU and high CFU early-detected granulomas. Each dot represents a granuloma. Box plot shows median, IQR and range. Statistics: non-parametric Mann Whitney U test. Source: Gideon et al., Pre-print
Dr Flynn and her collaborators have demonstrated that the bacterial burden in granulomas is very heterogeneous, with many granulomas eventually becoming sterile, while others remain active (Lin et al., 2014). Can we determine host immune responses associated with resolving (sterile) and permissive (M.tb growth and eventual dissemination) granulomas? Using a 10-week NHP TB infection experiment, they observed that granulomas established early (detectable using PET-CT by 4 weeks post-infection) are associated with a higher bacterial burden than granulomas established late (detectable at 10 weeks post-infection). Interestingly, cellular composition differed between early (high CFU) and late (low CFU) granulomas. Early granulomas had higher proportions of mast and plasma cells but lower proportions of CD4/CD8 T and natural killer cells than late granulomas. (Late) granulomas that facilitated bacterial killing contained significantly higher proportions of CD4+ and CD8+ T cells expressing hybrid Type1-Type17 (positive for transcription factors that define Th1 and Th17 cells) immune responses or stem-like features and CD8-enriched T cells with specific cytotoxic functions; failure to control correlated with mast cell, plasma cell and fibroblast abundance. Interestingly, the type1-type 17 cells expressed Th1 associated cytokines but not IL-17. However, Th1 cytokine expression levels were similar between early and late granulomas. Further, they showed that granulomas established early and better controlled M.tb replication had higher proportions of T1/T17 cells and cytotoxic (innate and adaptive immune) cells clusters than early granulomas that had high CFU by week 10.
Journal Article: Gideon et al., Pre-print. Single-cell profiling of tuberculosis lung granulomas reveals functional lymphocyte signatures of bacterial control. bioRxiv
Summary by Cheleka AM Mpande










