- Patient presentation
- History
- Differential Diagnosis
- Examination
- Investigations
- Discussion
- Treatment
- Final outcome
- Evaluation - Questions & answers
Patient presentation
A 14 and half year old boy presents with a recent history of tender temperomandibular joints and regular morning stiffness in both hips. He has a limited range of movement in his hips, especially abduction and adduction, and is no longer able to run and play games with his brothers.
Acknowledgement
This case study was kindly provided by Dr Monika Esser MMed Paed, Head of Division of Immunology, N.H.L.S Coastal Branch, Tygerberg Hospital.
Partnership
We have partnered with The International Union of Basic and Clinical Pharmacology (IUPHAR) to bring you in-depth information about drugs and pharmacology with links to the Guide to ImmunoPharmacology.
History
14 years old
- Our patient started suffering with painful hips from age 14 and within a month he was unable to walk unassisted. The pain presented with the typical features of an inflammatory response i.e. worse in the morning and improving with activity during the day.
- Minimal relief was obtained from paracetamol.
- Associated features included occasional fevers, malaise, weight loss, no skin rashes, no urogential symptoms and no visual impairment.
Focused past medical history
- Intermittent pain in the left and right groin for the past 2 years.
- Age 11 yrs he had uncomplicated nephritis.
- Age 10 yrs he had severe Infectious Mononucleosis.
- Treatment for moderate asthma as a young child.
Family History
2 older male siblings both enjoy good health. No family history of Psoriasis or chronic skin rashes.
Allergies
Aspirin
Differential Diagnosis
- Reactive arthritis eg Reiters syndrome
- Oligoarticular JIA
- Ankylosing spondylitis
- Psoriatic subtype
Examination
Patient was referred to the orthopaedic service where on examination he appeared chronically ill with a weight of 43.2kg (25th centile) and a height of 158cm (25-50th centile). General examination was normal. No signs of jaundice, anaemia, cyanosis, clubbing, oedema or lymphadenopathy.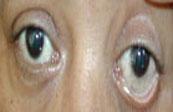 Musculoskeletal examination showed the patient was:
Musculoskeletal examination showed the patient was:
- Unable to bear weight on his legs.
- Quadriceps muscles were severely atrophied.
- Bilaterally he had very tight iliotibial bands.
- Passive movement of both hips showed reasonable ranges of movement in all directions but active movements were difficult to assess because of severe pain.
- Loss of normal lumbar lordosis as seen pictured.
- No evidence of uveitis
- Ankylosing Spondyitis patient and a patient exhibiting early uveitis pictured.
Investigations
| Initial Investigations | |
|---|---|
| C-reactive Protein | 3 (Normal |
| ESR | 28mm/hour (Normal 1-13mm/hour) |
| WBC | 6.6 (Normal |
| Hb | 12.5 g/L (Normal) |
| Bone isotype scan showed increased uptake in the left calcaneal region. | |
| 3 weeks after no improvement on traction and analgesics more tests were ordered. | |
| Further Investigations | |
| Rheumatoid factor | Negative |
| HLA B27 | Positive |
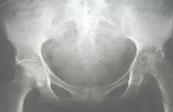
| X-rays | Showed beginning of fusion of sacroiliac joints and early signs of destruction of the left hip joint. |
Discussion
The spondyloarthropathies are a family of related disorders that include ankylosing spondylitis (AS), reactive arthritis (Reiter’s syndrome), psoriatic arthritis (PsA) and spondyloarthropathy associated with inflammatory bowel disease (IBD), to name a few. They are linked by common genetics, the human leukocyte antigen HLA-B27 and a common pathology, enthesitis. Ankylosing spondylitis was the first of the spondyloarthropathies to be linked with an HLA gene.
The spondyloarthropathies are chronic inflammatory diseases involving the sacroiliac joints, axial skeleton, and to a lesser degree, peripheral joints and extra-articular organs which includes the eyes, skin, and cardiovascular system. The etiology is unknown but involves the interaction of genetic and environmental factors. Some of these factors relating specifically to Ankylosing Spondylitis are discussed below.
Various hypotheses to explain the cause of ankylosing spondylitis include thymic abnormalities, bacterial superantigens, antibodies to HLA-B27, HLA-B27 derived peptides or aberrant folding of HLA-B27 receptors. The most likely explanation is the “arthritogenic peptide” hypothesis involving HLA-B27 receptors. This speculates that the tissue damage seen in the joints of ankylosing spondylitis patients is mediated by HLA-B27 restricted CD8+ Cytotoxic T Lymphocytes responding to “self”-antigens expressed in joint tissue. In addition, it is thought that the autoreactive T cells are generated in response to a primary infection with intracellular bacteria that produce proteins that share highly similar or identical peptide antigens to cellular proteins “molecular mimicry”. These peptides are processed via the endogenous antigen sampling pathway and bind specifically to certain subtypes of HLA-B27 class I MHC receptors expressed on the surface of joint tissue cells, most commonly HLA-B2702, HLA-B2704, HLA-B2705, HLA-B2707 and HLA-B2708. Other subtypes such as HLA-B2706 and HLA-B2709 are not associated with the disease. Non-HLA-B27 class I alleles have also been reported to be involved such as HLA-B1403, HLA-B39 and HLA-B60. This supports the “self”-peptide binding hypothesis, since the alleles that contribute to the disease most likely share common peptide-binding motifs (and fall into a family known as HLA supertypes). It is therefore highly probable that CD8+ Cytotoxic T Lymphocytes that recognize these HLA class I molecules along with the peptides derived from the bacterial antigens cause aberrant immune attack to the surface of joint tissue cells.
Although the bacterial proteins and human cellular proteins involved in the autoimmune response are yet to be identified there are reasons to support the involvement of intracellular bacteria in the initiation of the autoimmune response. It is known that bacteria such as Salmonella, Shigella, Yersinia, Campylobacter, Chlamydia, Mycobacteria and possibly Brucella can trigger reactive arthritis. These bacteria can survive intracellularly which is a requirement to generate a CD8+ Cytotoxic T lymphocyte response, although at the time of onset of the symptoms of ankylosing spondylitis, no bacteria are usually present, indicating that the development of the disease is a delayed effect from a prior immune response. This stimulus includes the bacteria in the gastrointestinal tract. In studies of HLA-B27 transgenic rats in the presence of bacteria, the rats developed an illness similar to the spondyloarthropathies, with sacroiliitis, enthesitis, arthritis, skin and nail lesions, ocular involvement, and gastrointestinal tract involvement.
Also, in support of the “arthritogenic peptide” hypothesis, an in vitro study in ankylosing spondylitis patients has identified the presence of HLA-B27 restricted CD8+ Cytotoxic T Lymphocytes responding to “self”-peptides derived from collagen, a common protein found in joints, which demonstrates the possibility of causative role for Cytotoxic T lymphocytes in the development of the disease. Ongoing investigations are however needed to identify the bacterial equivalent of such peptide antigens.
Cytokines, in particular tumor necrosis factor-a (TNF- a) and transforming growth factor-beta (TGF-ß), are important in the inflammatory process by leading to fibrosis and ossification at sites of enthesitis.
Download images for this case
Treatment
The patient was put in traction for relief of painful hips, given analgesics and because of lack of improvement was referred to the rheumatology service after 3 weeks.
Intensive rehabilitation with hydrotherapy and physiotherapy with analgesia was commenced and the patient was able to walk with crutches and independently within a month.
Treatment with Methotrexate as a Disease Modifying Agent and low dose Prednisone were added to the analgesia and physiotherapy.
Download images for this case
Final outcome
Despite initial response to therapy over the following two years the patient developed:
- Progressive inflammatory joint involvement of knees, ankles and shoulders
- Enthesitis around the R knee
- Lower back pain with loss of normal lordosis and a CT scan confirmed erosions of both sacro-iliac joints and evidence of ankylosis of both hip joints. This development helped to confirm the patient’s diagnosis.
- Some relief was obtained from intra-articular steroid injections of both hips and patient was maintained on Methotrexate. (Within a more resourced background the patient would have qualified for TNF alpha blocker medication).
After 6 years:
- An orthopaedic evaluation revealed stiff ankylosis of both hips with sufficient mobility for a sedentary job.
After 8 years:
- Currently aged 22 years the patient is pain-free and is to be reviewed at regular intervals for a possible hip replacement.
- Opthalmic examinations have repeatedly remained negative for evidence of uveitis.
Download images for this case
Evaluation – Questions & answers
What is the diagnosis
Ankylosing spondylitis is inflammation of the spine and large joints, resulting in stiffness and pain. The disease is 3 times more common in men than in women, developing most commonly between the ages of 20 and 40. Its cause is unknown but there is a genetic and environmental link.
The symptoms include mild to moderate flare-ups of inflammation which generally alternate with periods of almost no symptoms. In Juvenile onset the typical symptoms may be pain and stiffness or objective inflammation of peripheral joints, especially of the lower extremities, and enthesitis at one or more sites around the knee or foot. Characteristic backpain may not be present then. The most common symptom in adults is back pain, which varies in intensity from one episode to another. Pain is often worse at night and in the morning with early morning stiffness that is relieved by activity. Pain in the lower back and associated muscle spasms are often relieved by bending forward which can result in a permanent stooped position.
Associated symptoms include:
- loss of appetite
- weight loss
- fatigue
- anemia
- costovertebral joints become inflamed, resulting in limited chest wall expansion on respiration
- pain may start in large joints, such as the hips, knees, and shoulders.
- one third of people have recurring attacks of uveitis.
- may develop inflammation of a heart valves which results in permanent damage.
- rare complication is cauda equine syndrome from spinal nerve compression.
How does the HLA association specific for Ankylosing Spondylitis (AS) vary among different racial groups?
> 90% of white AS patients
50 – 80% of non-white AS patients
Prevalence of HLA B27 allele in general population is:
8% in healthy whites
3% in healthy North American blacks
To what extent does positivity increase the relative risk of developing AS?
What is the MHC complex and where is it located?
What is meant by the term HLA?
How is HLA B27 hypothesized to play a role in the pathogenesis of AS?
What are some possible reasons for the mechanisms by which the MHC might confer this susceptibility?
What treatment options are available for AS?
- Nonsteroidal anti-inflammatory drugs (NSAIDs) can reduce the pain and inflammation, thus enabling people to do important exercises to retain posture, including stretching and deep breathing.
- Methotrexate is an antimetabolite drug which blocks the metabolism of cells.
- Sulfasalazine is an immunosuppressive drug for long-term reduction of inflammation for pain in joints.
- Tumor necrosis factor (TNF) inhibitors such as etanercept of infliximab for relief of pain and inflammation. These are newer drugs that have shown great promise in treating ankylosing spondylitis. Studies have shown that these drugs can potentially slow or even halt the progression of the disease.
- Corticosteroids for short-term treatment of inflammation of the eyes and of joints other than the spine.
- Muscle relaxants and opioid analgesics are usually used for only brief periods to relieve severe pain and muscle spasms.
- Joint replacement surgery for hips or knees that become eroded or fixed in a bent position.
- Physiotherapy
- Hydrotherapy
The long-range goals of treatment are to maintain proper posture and develop strong back muscles.
Download images for this case