According to a new study, immune cells like dendritic cells, which are essential for the immune system’s activation, recover more slowly the more serious the COVID-19 infection is (Figure 1). They were able to demonstrate that multiple different immune cell types were still negatively impacted six months after a severe COVID-19 infection. They found parallels between what occurs to immune cells in conditions including cancer and HIV, continuing immunological activation, and chronic infections in the body.
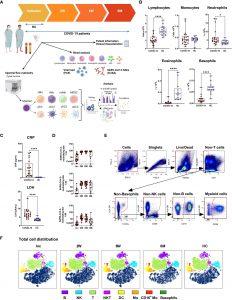
Figure 1: Study outline and experimental design. PBMCs and serum were collected from 21 COVID-19 patients and 16 healthy donors over a 6-7 month period. (A) Design of COVID cohort study illustrating timepoints for sample collection and experimental outputs, created with BioRender BioRender.com. Initial clinical assessments of (B) blood cell counts, (C) plasma C-reactive protein (CRP) and lactate dehydrogenase (LDH), and (D) neutralizing SARS-CoV-2 antibody titers. (E) Representative gating strategy to demonstrate live/dead gating and lineage exclusion, to leave myeloid cell populations for further analysis. (F) tSNE plots showing distinct clustering of all live cells, with 17 patients overlaid, and 16 controls overlaid. Data is represented as mean with 95% Cl, with significance of *p ≤ 0.05, ****p ≤ 0.0001, determined using Brown-Forsythe and Welch ANOVA tests. Inc, Study inclusion; 2W, 2 weeks; 6W, 6 weeks; 6M, 6-7 months; HC, healthy control. Mo, monocytes; cMo, classical; iMo, intermediate; ncMo, non-classical; MDSC, myeloid-derived suppressor cells; DC, dendritic cells; pDC, plasmacytoid; cDC1/2/3, conventional.
The innate immune system, which is required for the body to form any sort of particular immunological response at all, has been the focus of the researchers’ deeper examination in this work. The immune system must recognise a novel virus when it enters the body for the first time, as SARS-CoV-2 at the start of the epidemic. Dendritic cells, a kind of cell group, are required for this to occur. These in turn stimulate T cells that can destroy SARS-CoV-2-infected cells and B cells that can create antibodies that can neutralise the virus. In order to connect the innate and adaptive immune systems, dendritic cells are essential.
In their investigation, researchers found a relationship between the severity of an illness and its impact on dendritic cells. Additionally, it was demonstrated that six months later, there is still a difference in the distribution of the various monocyte subtypes among patients and the healthy control group. The change in monocytes, in particular in the lungs, suggests that the body is still healing from a significant sickness, according to the experts.
Journal article: Francis R. Hopkins, F.R., et al., 2023. Major alterations to monocyte and dendritic cell subsets lasting more than 6 months after hospitalization for COVID-19. Frontiers in Immunology.
Summary by Stefan Botha










