Shiga-toxin (Stx) producing enterohaemorrhagic E.coli (STECs) have been implicated in outbreaks of hemolytic uremic syndrome (HUS). HUS is life threatening disease characterized by haemolytic anaemia, thrombocytopenia (low platelet count) and uremia (acute kidney injury/failure). To date no therapy against HUS, highlighting the need for increased research in this area.
Research on HUS has suggested a potential immunopathological contribution by monocyte to HUS pathology. Monocytes subsets in the blood can be distinguished by differential expression of CCR2 and Gr1. Researchers aimed to determine the contribution of Gr1high monocytes during HUS.
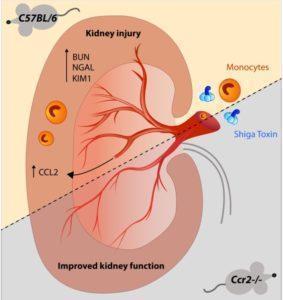
Pohl et al., used an used an experimental mouse model of HUS. Mice were intravenously injected with Stx and LPS, this resulted in increased blood urea nitrogen (BUN) and other symptoms characteristic of acute kidney injury. Acute HUS (1 day post Stx/LPS injection) resulted in increased levels of renal monocytes Gr1high expressing high levels of CD11b and were CX3CR1lowMHC ClassII–CD64high. Using non-invasive imaging techniques researchers observed extensive kidney damage which was associated with increased levels of Gr1high monocyte.
HUS has also been associated with increased levels of chemokines CCL2, CCL3 and CCL5, that that recruit monocytes via the chemokine receptor CCR2. High expression of CCR2 on Gr1high monocytes suggested that CCR2 is required for Gr1high monocytes to contribute to immunopathology. Indeed Pohl et al., demonstrated that in absence of CCR2 there was a reduction on recruitment of Gr1high monocytes, this was associated with reduced kidney damage and increased survival.
The research conducted by Pohl et al., showing mechanism by which CCL2 via CCR2 contributes to Stx induced HUS immunopathology by recruiting Gr1high monocytes, cells that contribute to HUS immunopathology.
Journal Article: Pohl et al., 2018. CCR2-dependent Gr1high monocytes promote kidney injury in shiga toxin-induced hemolytic uremic syndrome in mice. European Journal of Immunology.
Article by Cheleka AM Mpande