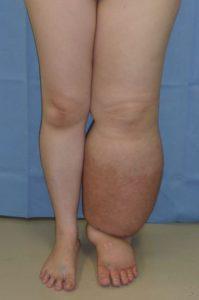
Lymphedema is a condition which affects the functioning of the lymphatic system resulting in swelling usually in the arms or legs. The condition has traditionally been managed through non-pharmacological therapies, however these therapies cannot cure the condition. Researchers have identified an anti-inflammatory drug, ketoprofen, that reversed pathology in mouse models of lymphedema through the antagonism of the pro-inflammatory mediator leukotriene B4 (LTB4). This metabolite may therefore be a good target for the development of less toxic and more specific lymphedema drugs.
The lymphatic system is an important component of the immune system. It includes the lymph nodes, spleens, tonsils, thymus, adenoids and lymph vessels throughout the body. Lymphocytes are produced in the lymphoid organs and the lymph transports cells such as dendritic cells to the lymphoid organs to present antigens and stimulate an immune response. The lymphatic system is also responsible for transporting fat, transporting lymphocytes around the body and removing interstitial fluid before it accumulates in the tissues. Lymphedema is a dysfunction of the lymphatic system resulting in the retention of lymphatic fluid in the tissues which results in edema.
Whilst secondary lymphedema can usually be attributed to a certain trigger or cause, for example, removal of lymph nodes during breast cancer surgery, the causes of primary lymphedema are not well understood. Currently, there is no cure for lymphedema and individuals with the condition manage it by a variety of methods such as manual lymphatic drainage and wearing compression garments. Researchers from the Stanford University School of Medicine found that ketoprofen, an anti-inflammatory drug, reduced lymphedema symptoms. They then wanted to determine the mechanisms behind this.
The team used a mouse model of lymphedema in which mouse tail lymphedema closely resembles the pathology and immune characteristics of human lymphedema. The researchers found that the effects of ketoprofen were due to the inhibition of LTB4. LTB4 is produced by leukocytes and is involved in the inflammatory response. It recruits and activates neutrophils, monocytes as well as eosinophils and has been shown to stimulate the secretion of pro-inflammatory cytokines. Unfortunately,the ketoprofen drug has many side effects including hepatic toxicities and therefore is not a good candidate for lymphedema treatment.
Inhibition of the LTB4 metabolite by bestanin, a protease inhibitor and less toxic drug than ketoprofen, resulted in improved lymphatic functioning and decreased swelling of the mouse tails. Bestatin was also found to limit macrophage inflammation. The concentration of LTB4 rose during lymphedema progression and LTB4 synthesis was higher in individuals with lymphedema as opposed to controls.Using cell-based assays, the researchers found that higher concentrations of LTB4 induced apoptosis of human lymphatic endothelial cell. Higher concentrations of LTB4 inhibited both Notch pathways and vascular endothelial growth factor receptor 3 in these cells. The researchers found that the maintenance of lymphedema symptoms was controlled by the inhibition of Notch signalling in the lympathic system by LTB4.
In summary the researchers found that ketoprofen works by inhibiting LTB4. LTB4 increases the pathogenesis of lymphedema and therefore development of drugs specific for the condition may need to focus on this pro-inflammatory mediator.
Journal article: Tian et al., 2017. Leukotriene B4 antagonism ameliorates experimental lymphedema. Science Translational Medicine
Article by Thandeka Moyo