Hereditary angioedema (HAE) is a rare inherited disorder characterised by recurrent, unpredictable swelling episodes that can affect the abdomen, limbs, face, genitals, and upper airways. These attacks can be painful and, in some cases, life-threatening. Without effective treatment, the condition can significantly reduce quality of life. Although research over the past decade has led to the development of more targeted therapies and updated international treatment guidelines, many patients still do not achieve optimal disease control. One reason is that interpreting and implementing these guidelines in everyday clinical practice can be challenging, leading to variations in care across healthcare settings.
The burden of HAE extends beyond the physical symptoms of swelling. Patients often experience psychological stress, social limitations, and economic impacts associated with the condition. Many report missing work, school, or important life events due to attacks. Even when attack frequency is relatively low, the unpredictability of episodes can create ongoing anxiety and fear, affecting well-being between attacks. For families in which multiple members are affected, the overall burden can be even greater.
Current management strategies for HAE includes several therapeutic approaches. On-demand treatment (ODT) is used to control acute attacks and should be administered as early as possible. Approved ODT options in Europe include oral sebetralstat as well as injectable therapies such as icatibant and plasma-derived or recombinant C1 inhibitor. While these treatments are essential for managing acute episodes, they do not prevent future attacks, meaning that patients relying only on ODT may continue to experience substantial disease burden.
Preventive strategies play a key role in improving long-term outcomes. Short-term prophylaxis (STP) may be used to prevent attacks in situations with increased risk, such as surgical or dental procedures. Long-term prophylaxis (LTP) aims to reduce the frequency and severity of attacks over time and is recommended for many patients. First-line LTP therapies for adolescents and adults now include agents such as berotralstat, C1 inhibitor therapy, and lanadelumab, with newer options including garadacimab and donidalorsen. These therapies are available in multiple formulations, oral, intravenous, and subcutaneous, allowing treatment to be tailored to individual preferences and lifestyles. Earlier treatments such as attenuated androgens are now used far less frequently due to safety concerns, and antifibrinolytics are generally not recommended because of limited evidence of effectiveness.
According to international guidelines published by the World Allergy Organization and the European Academy of Allergy and Clinical Immunology, the ultimate goal of HAE treatment is ambitious: achieving full disease control and restoring a normal life for patients. Reaching this goal typically requires long-term prophylaxis, which should be considered for every patient and regularly reassessed during clinical visits. However, translating guideline recommendations into consistent clinical practice requires practical strategies that help clinicians apply them effectively.
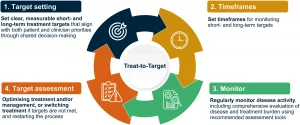
One proposed solution is the adoption of a Treat-to-Target (T2T) approach in HAE management (Figure 1). T2T focuses on defining clear, personalised treatment goals and monitoring progress toward those goals over time. If targets are not achieved, treatment can be adjusted or optimised. This approach emphasises shared decision-making between clinicians and patients, structured monitoring of disease activity and quality of life, and continuous evaluation of treatment effectiveness.
Originally developed in cardiology, the T2T strategy has proven successful in improving outcomes in several chronic and immune-mediated diseases, including rheumatoid arthritis, psoriatic arthritis, and diabetes. Applying similar principles to HAE may help standardise care, support more consistent implementation of treatment guidelines, and ultimately enable more patients to achieve the goal of living a normal, attack-free life.
Journal article: Cancian, M., et al. 2026. A Treat-to-Target approach in hereditary angioedema: expert consensus from a European committee. Frontiers in Immunology.
Summary by Stefan Botha