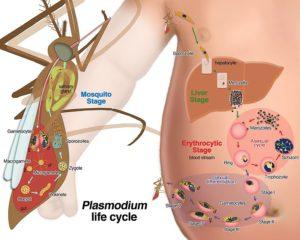
Malaria is still a major global health problem affecting large numbers of people mostly in developing countries. Malaria is caused by the Plasmodium parasite which is transmitted to humans through the female Anopheles mosquito. The highest mortality related to malaria infection is in children under the age of 5 years old and therefore better drugs and improved vaccines need to be developed.
Burkina Faso is a malaria endemic West African country with an estimated 15 000 malaria-related deaths in 2015, according to the World Health Organization. Artemisinin combination based therapy (ACT) has become the recommended first line of treatment for people with uncomplicated malaria in Burkina Faso. ACT has proven to be effective in the clearance of parasites and in the reduction of fever.
Fatimata Thiombiano from Burkina Faso presented her data at the International Remote Conference on the effect ACT treatment has on antibody responses in both children and adults. The researchers are part of WANECAM, which is a multi-centric study in Burkina Faso, Mali and Ghana looking at the efficiency and safety of ACT.
In previous studies to determine immune response to malaria after ACT treatment, malaria-infected mice were treated with ACT and its derivatives and their immune responses were monitored. It was found that the mice had decreased cytokine production from Il6 to Il12, lower IFN-gamma production and lower antibody response to malaria.
The next step, conducted by Thiombiano and colleagues, was investigate whether this effect was also seen in humans. The researchers included consenting participants who had a fever, had not taken anti-malarial tablets in the last two weeks, had trophozoite numbers less than 200000/ul blood and were able to take the oral ACT.
The participants were started on treatment and the researchers took blood samples on the first day of the study and 28 days later. The blood was used for blood smears to check parasitaemia and was also used to obtain antibody-containing serum.
The researchers found that ACT worked efficiently in reducing the amount of parasites in the participants and decreased the symptoms of malaria. The amount of malaria-specific antibodies did not change significantly over the 28 days of treatment when all participants were grouped together. However, when divided into the different age groups, malaria-specific antibody responses increased significantly from Day 0 to Day 28 for children under the age of 5.
This study suggests that the antibody responses to malaria may not be affected by ACT treatment. Understanding the immune response towards malaria parasites may be an essential first step in developing effective therapeutics against the disease.
For more information on the conference visit: 2nd Annual International Remote Conference: Science and Society
Article by Thandeka Moyo